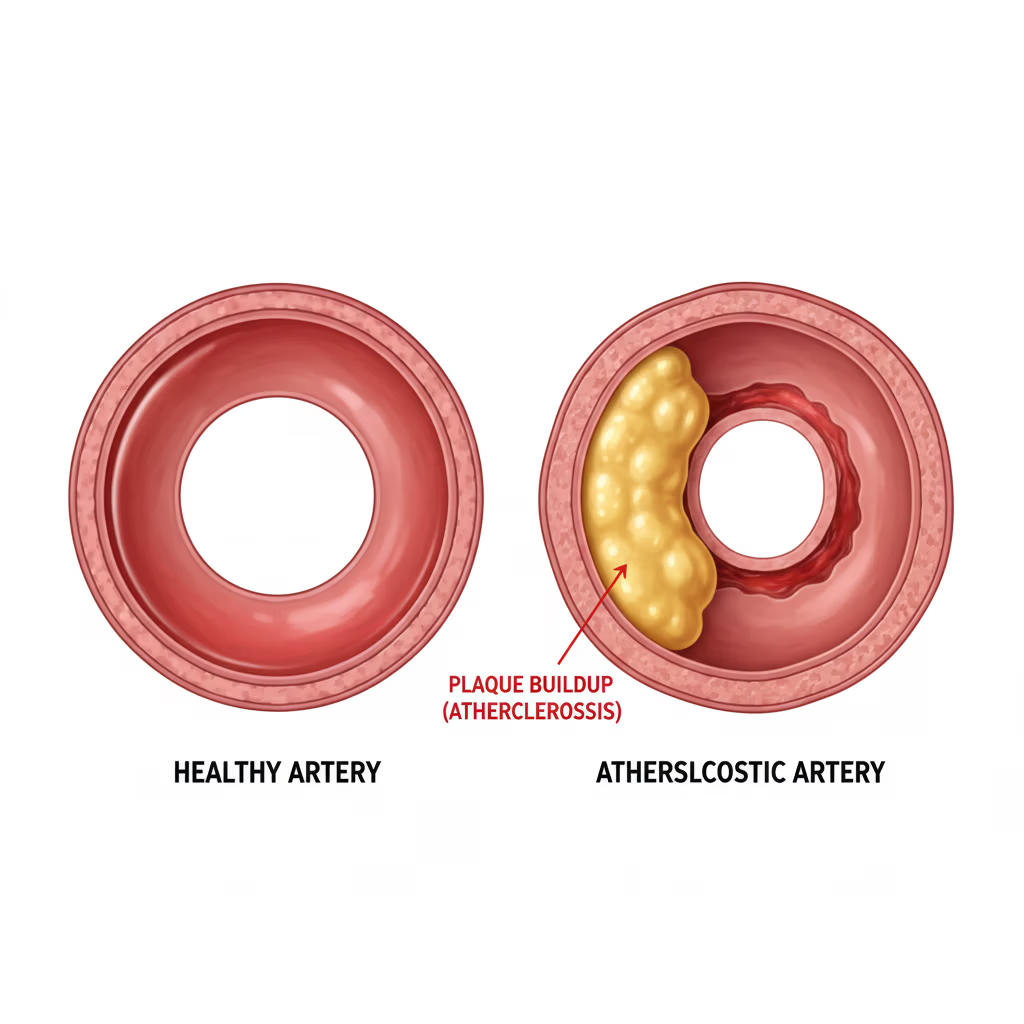
Peripheral Vascular Disease (PVD) is a slow and progressive circulation disorder. It can be caused by the narrowing, obstruction, or spasms of the blood vessels.
This disease affects any blood vessel outside of the heart, including arteries, veins, or lymphatic vessels. However, the legs and feet are most commonly affected. Organs supplied by these vessels, such as the brain and the extremities, may not receive enough blood flow to function correctly.
Causes
The most common cause of PVD is atherosclerosis, which is the buildup of plaque inside the arterial walls. This accumulation reduces the space through which blood flows, leading to decreased oxygen and nutrients available to tissues and organs. Furthermore, this buildup can trigger blood clots, further obstructing the body’s main arteries.
Other causes of PVD include:
-
Injuries to arms or legs.
-
Irregular muscle or ligament anatomy.
-
Infections.
It is often observed that individuals with Coronary Artery Disease (CAD) also suffer from PVD.
Risk Factors
Factors you cannot change:
-
Age: Especially those over 50.
-
History of heart disease.
-
Gender: Males and postmenopausal women.
-
Family history: High cholesterol, high blood pressure, or PVD.
Factors you can change or treat:
-
Coronary Artery Disease (CAD).
-
Diabetes.
-
High cholesterol and High blood pressure (Hypertension).
-
Excess weight or obesity.
-
Physical inactivity.
-
Smoking or tobacco use.
Note: Individuals who smoke or have diabetes have the highest risk of complications because these factors significantly impair blood flow.
Symptoms
Approximately half of those diagnosed with PVD show no symptoms. For those who do, the most common first sign is intermittent claudication (painful leg cramps during exercise that are relieved by rest).
Other symptoms include:
-
Skin changes: Decreased skin temperature or thin, brittle, shiny skin on legs and feet.
-
Weak pulses in legs and feet.
-
Gangrene: Dead tissue due to lack of blood flow.
-
Hair loss on the legs.
-
Impotence (Erectile dysfunction).
-
Non-healing wounds over pressure points (heels or ankles).
-
Numbness, weakness, or heaviness in muscles.
-
Burning pain at rest, commonly in the toes and at night.
-
Paleness when legs are elevated or blue-red discoloration of extremities.
-
Thickened, opaque toenails.
Diagnostic Tests
Beyond a physical exam and medical history, the following tests are used to diagnose PVD:
-
Angiograms: X-rays using contrast dye to find blockages.
-
Ankle-Brachial Index (ABI): A comparison of blood pressure in the ankle vs. the arm.
-
Doppler Ultrasound: Uses sound waves to evaluate blood flow.
-
Magnetic Resonance Angiography (MRA): A non-invasive test using magnets and radio frequencies to see vessels.
-
Treadmill Exercise Test: Monitoring circulation while walking.
-
Photoplethysmography (PPG): Uses infrared light to evaluate blood flow near the skin surface.
-
Pulse Volume Recording (PVR): Calculates changes in blood volume in the legs.
-
Reactive Hyperemia Test: Used for patients unable to walk on a treadmill.
Treatment and Prevention
Treatment focuses on managing symptoms and stopping disease progression to reduce the risk of heart attack and stroke.
Prevention and Lifestyle Changes:
-
Quit smoking: Including secondhand smoke.
-
Healthy Diet: Reduce fats and simple sugars; increase fruits, vegetables, and lean proteins.
-
Exercise: At least 30 minutes a day.
-
Weight Management: If overweight, consult your doctor for a plan.
-
Chronic Disease Management: Strictly follow treatments for diabetes, hypertension, and high cholesterol.
-
Medications: Always take blood thinners or wall-relaxing medications as prescribed.
Complications of untreated PVD: Amputation, chronic pain, restricted mobility, and a significantly higher risk of stroke.
